Tuvaluan community drives message to improve skin infection rates
A community-driven approach has played a vital role in a project that has reduced the rate of skin and soft tissue infections among under 25-year-olds in West Auckland’s Tuvaluan community by more than 40 percent.
A large proportion of Auckland’s Tuvaluan community live in the area served by health and social services provider, The Fono.
Clinical director and project lead, Dr John Kennelly, was concerned that skin infections have been on the rise in the Tuvaluan community since 2013, even though overall rates in Pacific communities have declined.
Staphylococcus aureus is bacteria that is naturally present on healthy skin, but if the skin is broken because of conditions like eczema, scabies or a cut, the bacteria can get into the bloodstream and become life threatening.
‘Poverty sometimes results in multiple families living together in cramped conditions which increases the likelihood of infection,’ says John.
‘There was an overwhelming feeling that this problem was totally out of control, and we knew that treating one individual after another as they came through my room was not the answer.’
And so, the ‘Happy skin’ project was developed with the aim of reducing the rate of skin and soft tissue infections in the community by 25 percent.
The project was undertaken as part of the 2018 Whakakotahi quality improvement programme, which aims to increase quality improvement capability in primary care and support the key focus areas of equity, integration, consumer engagement and consumer co-design.
Successful providers are supported by the Commission to implement quality improvement projects in an area of patient care that is important to their patients or community and to them as providers.
The Commission’s primary care programme team supports and mentors participating teams through site visits and group learning events. A member of each project team has also been offered a position on the primary care quality improvement facilitator course delivered by Ko Awatea and the Commission's primary care and leadership capability programmes.
‘We adopted an ‘action research approach’, where the participants become the researchers,’ says John.
‘We went to the Tuvaluan community and asked them what they wanted us to do to help them solve this problem.’
He says taking the message to churches was key to the project’s success.
‘Church is the equivalent of a marae for the Tuvaluan community. Even if someone’s not there on the day, other family members will get the messages out and it spreads like wildfire – in a good way!
‘While we did some trouble shooting and gave them some ideas, the community came up with the solutions. Leaders are found in all walks of life and they aren’t always the people in charge.
‘The Tuvaluan community’s collective culture is an absolute strength because it means that when they make a decision, they make it together. There’s a real closeness and intelligent communication.
‘I knew a lot of them, of course, and we have a Tuvaluan nurse who translated the medical messages for me. Then, several of their wonderful speakers used their authority in the church to motivate people to fix the problem.
‘They even wrote a ‘Happy skin’ song because, for the Tuvaluan community, any occasion is an opportunity to sing.’
Key messages included the importance of washing hands and dishes properly, and reporting sores early so they can be treated.
‘We set up a system where community workers would take a photo of a boil and text it to me and I’d prescribe the treatment on the spot.’
Over the nine-month project, the rate of skin infections dropped more than 40 percent from an initial average of 24 per 1000 patients to 14 per 1000, well in excess of the target.
The equity gap also decreased between the Tuvaluan population and other Pacific groups from 9 per 1000 patients to 5 per 1000, and from 16 per 1000 to 9 per 1000 for non-Pacific groups.
The project’s improvement facilitator, Janet Tekori, agrees it was successful because it was driven by the community.
‘We’re proud of our result and the raised awareness of the problem. We now see fewer patients with skin and soft tissue infections in our clinic. Our board has now directed us to prioritise the project and use the learnings for the wider patient group.’
She says the project team, which donated a lot of time, enjoyed being part of Whakakotahi 2018, meeting the other project teams and sharing learnings.
‘We were very grateful for the Commission’s support, particularly quality improvement advisor Jane Cullen, who consistently followed up with us to ensure we were on track.’
John says Janet’s role allowed him to take a step back and focus on data gathering and examination. John is a senior lecturer in the University of Auckland’s school of population health’s department of general practice and primary health care.
‘I’ve had a long association with people there and we’re good at collecting data from the electronic medical record, so I felt confident we had the data. I was assisted by former colleague, researcher Dr Helen Gu, who, although she is now based in the United States was keen to help process the data. I couldn’t have done this without her.’
Dr John Kennelly and Janet Tekori are presenting their project on Saturday 27 July 2019 at the Royal New Zealand College of General Practitioners conference in Dunedin, supported by Jane Cullen.
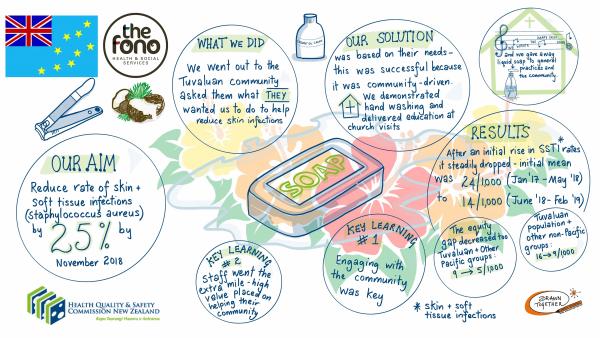
An infographic outlining the community-driven project to improve skin infection rates. Download a copy of the graphic (1.1MB, JPG
