Update on anti-staphylococcal bundle using a collaborative approach
Over the past year the Health Quality & Safety Commission’s infection prevention and control programme team has facilitated the implementation of a preoperative anti-staphylococcal bundle within the Surgical Site Infection Improvement (SSII) Programme.
This bundle aims to reduce the Staphylococcus aureus SSI rate by implementing a bundle of well-established interventions to reduce the SSI risk for cardiac and orthopaedic surgery. The Commission worked with interested hospital teams to roll out the bundle using a collaborative and quality improvement methodology. A total of eight hospital teams (five district health boards [DHBs] and three private hospitals) implemented a bundle.
Participating organisations
| Hospital | Specialty scope |
| Acurity Health – Bowen Hospital | Orthopaedic |
| Acurity Health – Wakefield Hospital | Both |
| Auckland DHB | Cardiac (adult patients) |
| Lakes DHB | Orthopaedic |
| Southern Cross – Hamilton Hospital | Both |
| Southern DHB | Cardiac |
| Waikato DHB | Cardiac |
| Waitemata DHB | Orthopaedic |
During the 10-month-long collaborative, small groups (2–4 people per hospital team) attended 3 face-to-face learning sessions with additional members working on improvements in each organisation. Monthly webinars and individual team teleconferences were held. The Commission’s infection prevention and control senior advisor provided additional training related to quality improvement methodology, information sharing and clinical discussion. The multidisciplinary teams involved in the collaborative were highly engaged and well supported by the Commission and their local management throughout the implementation process.
All hospitals achieved 95–100 percent compliance for their bundle interventions. We will maintain contact with the project leads from each team to verify bundle compliance is sustained.
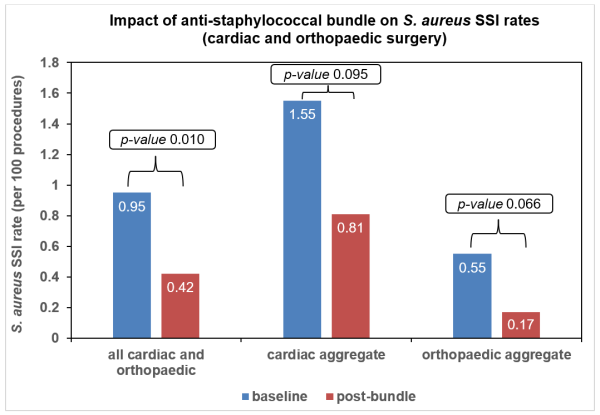
To date the bundle has been applied to nearly 3,000 procedures. Six months of preliminary data, post-implementation of the bundle, indicates there has been an aggregated 56 percent reduction in S. aureus SSI rates (p-value = 0.010) among the 8 participating hospitals for all operations (orthopaedic and cardiac).
For orthopaedic surgery, the 2 DHBs and 3 private hospitals that implemented a bundle had a combined pre-implementation Staphylococcus aureus SSI rate of 0.6% and post-implementation rate of 0.2% (p-value = 0.066). For cardiac surgery, the 3 DHBs and 2 private hospitals that implemented a bundle had a combined pre-implementation Staphylococcus aureus SSI rate of 1.6% and post-implementation rate of 0.8% (p-value = 0.095).
The graph below represents the combined S. aureus SSI rate pre- and post-bundle implementation for orthopaedic and cardiac surgery.
An educational video specific for surgical patients was developed. This video provides reminders for patients of things they can do to reduce their risk of an SSI before and after surgery. It was also translated into te reo Māori and Samoan. It is available for all hospitals to use for any surgical specialty as it is not targeted for just cardiac or orthopaedic surgical patients. The videos are located at here.
The Commission will continue to collect and analyse outcome data to determine the impact of the bundle on S. aureus SSI rates. We will provide further updates as we continue to assess the impact of the bundle. If the bundle is shown to have a significant and sustained impact, we will explore opportunities to implement the bundle in other hospitals and for other appropriate procedures.
Questions related to this update can be sent to SSIIP@hqsc.govt.nz.
