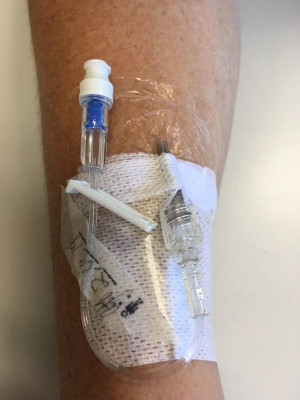
PIVCs are the most commonly used invasive medical device in health care. PIVCs are used for therapeutic purposes such as giving medicine, fluids and blood products.
At any time, over half of all patients in Aotearoa New Zealand hospitals will have a PIVC in situ. However, these devices do pose a risk to the patient and should only remain in place if they are required for the ongoing delivery of care.
Infections associated with a PIVC can be localised in the tissue around the entry site or spread to the bloodstream. At least one in four HA-SAB events in patients in our hospitals are linked to a PIVC.
A 24-month review of HA-SAB events in Aotearoa New Zealand identified that medical devices were the source for three-quarters (70.1 percent) of all HA-SAB events.
Read the report: Healthcare-associated Staphylococcus aureus bacteraemia: Te Whatu Ora – Health New Zealand districts.
PIVC quality improvement initiative
The infection prevention and control team at Te Tāhū Hauora is working on a quality improvement initiative to reduce infections associated with a PIVC.
In May 2023, we held four regional workshops to discuss PIVC management in Aotearoa New Zealand as part of scoping for the initiative. Fifty-five clinicians with an interest in reducing PIVC infections attended the workshops. Workshop participants shared local PIVC quality improvement initiatives and discussed factors contributing to PIVC-associated infections and ideas for improvement.
In August 2023, Te Tāhū Hauora invited clinicians to take part in a survey on PIVC management in Aotearoa New Zealand using an interactive platform called ThoughtExchange. A total of 216 participants took part. This enabled us to reach a broader range of clinicians and those who could not attend the workshops.
Results of the workshops and ThoughtExchange were presented at the Intravenous Nursing New Zealand conference in March 2024. The presentation can be viewed here: IVNNZ 2024 conference presentation (2.4MB, pdf).
A PIVC advisory group was established in August 2023 to provide sector leadership, advice and support to the initiative. The advisory group and Te Tāhū Hauora have developed a PIVC infection prevention bundle for adults. Te Tāhū Hauora is currently working on supporting resources for this bundle.
Look out for updates on this webpage and in our IPC newsletter.
For any questions, please contact the IPC team at IPC@hqsc.govt.nz.
Poster: HA-SAB Engagement using ThoughtExchange (PDF).
Poster: HA-SAB What are we going to do about increasing rates (PDF).

