You can download the full January–March 2019 QSM results (2.3 MB, PDF) or view the commentary and interactive charts below.
Local DHB report
Falls
Process marker 1: Percentage of older people assessed for the risk of falling
Nationally, 89 percent of older patients* were assessed for their falls risk in quarter 1, 2019. The rate has remained around the expected achievement level of 90 percent since quarter 4, 2013, despite some variations in a few quarters. At the district health board (DHB) level, 10 out of 20 DHBs achieved the expected marker level. Capital & Coast, Hutt Valley, Southern, Taranaki and West Coast DHBs have seen declines in assessments, while Bay of Plenty and Whanganui DHB have seen improvements.
Falls T 1
- Upper group: ≥ 90 percent
- Middle group: 75–89 percent
- Lower group: < 75 percent
* Patients aged 75+ (55+ for Māori and Pacific peoples)
Process marker 2: Percentage of older people assessed as at risk of falling who received an individualised care plan that addresses these risks
About 91 percent of patients assessed as being at risk of falling had an individualised care plan completed. This measure has increased 14 percentage points compared with the baseline in quarter 1, 2013. Achievements at DHB level vary but, overall, where patients have been assessed to be at risk of falling, completion of individualised care plans for that population group need to be at a consistently high level. In quarter 1, 2019, there were 14 DHBs in the upper group. MidCentral, Southern and West Coast DHBs have seen a decline in the development of an individualised care plan, while Bay of Plenty, Capital & Coast and Nelson Marlborough DHBs have seen an improvement.
Falls T 2
- Upper group: ≥ 90 percent
- Middle group: 75–89 percent
- Lower group: < 75 percent
When assessments and care plans are plotted against each other, a trend of movement over time is shown from the bottom left corner (low assessment and individualised care plan) to the top right corner (high assessment and individualised care plan). Five DHBs sat at the top right corner in quarter 1, 2013; in quarter 1, 2019, 10 DHBs are in this ‘ideal’ box (see Figure 3), down from 11 DHBs the last quarter. Auckland, Southern and West Coast DHBs are in the lower left corner, which is below the target for assessment and care plan.
Falls T 3
Outcome marker: In-hospital falls resulting in a fractured neck of femur per 100,000 admissions
There were 93 falls resulting in a fractured neck of femur (broken hip) in the 12 months ending March 2019.
To control the impact of changes in the number of admissions per month, Figure 4 shows in-hospital falls causing a fractured neck of femur per 100,000 admissions. The median of this measure was 12.6 in the baseline period of July 2010 to June 2012. It has moved down since September 2014, to 9.5 per 100,000 admissions, and shown a significant improvement. There was a high number of falls in February to October 2018. While this would normally be an indication of a significant increase in the rate, the subsequent months see a return to the median.
Falls T 4
The number of 93 in-hospital falls resulting in a fractured neck of femur is significantly lower than the 112 we would have expected this year, given the falls rate observed in the period between July 2010 and June 2012. The reduction is estimated to have saved $0.9 million in the year ending March 2019, based on an estimate of $47,000[1] for a fall with a fractured neck of femur.
We know some of these patients are likely to be admitted to aged residential care on discharge from hospital, which is estimated to cost $135,000 per occurrence[2].
If we conservatively estimate that 20 percent of the patients who avoided a fall-related fractured neck of femur would have been admitted to an aged residential care facility, the reduction in falls represents $1.2 million in total avoidable costs since March 2018.
Falls T 5
Hand hygiene
National compliance with the five moments for hand hygiene remains high.
Process marker 1: Percentage of opportunities for hand hygiene taken
National compliance with the five moments for hand hygiene remains high. Nationally, DHBs maintained an average of 86 percent compliance for the period November 2018–March 2019 compared with 62 percent in the baseline in July–October 2012.
HH T 1
- Upper group: ≥ 70 percent before quarter 3, 2014, 75 percent in quarters 3 and 4, 2014, and 80 percent since quarter 1, 2015.
- Middle group: 60 percent to target.
- Lower group: < 60 percent.
- Hand hygiene national compliance data is reported three times every year, not quarterly.
Outcome marker: Healthcare associated Staphylococcus aureus bacteraemia (SAB) per 1,000 bed-days
Healthcare associated SAB can be associated with medical devices or surgical procedures which means the onset of symptoms may occur outside of the hospital (community onset).
Figure 7 displays the monthly healthcare associated SAB per 1,000 bed-days. The final month is omitted, due to denominator completeness issues. From May 2017, the median has significantly increased from 0.11 to 0.13 per 1,000 bed-days. We are working with DHBs to better understand this shift and will monitor closely in the coming quarters.
HH T 2
Surgical site infection improvement (SSII) – orthopaedic surgery
As the Commission uses a 90-day outcome measure for surgical site infection (SSI), the data runs one quarter behind other measures. Information in this section relates to hip and knee arthroplasty procedures from quarter 3, 2013 to quarter 4, 2018.
Process marker 1: Antibiotic administered in the right time
For primary procedures, an antibiotic should be administered in the hour before the first incision (‘knife to skin’). As this should happen in all primary cases, the threshold is set at 100 percent. In quarter 4, 2018, 98 percent of hip and knee arthroplasty procedures involved the giving of an antibiotic within 60 minutes before knife to skin. Twelve DHBs achieved the national goal. In quarter 4, 2018 Counties Manukau Health has moved to the middle group. Northland DHB remains in the lower group.
SSII OS T 1
- Upper group: 100 percent
- Middle group: 95–99 percent
- Lower group: < 95 percent
Process marker 2: Right antibiotic in the right dose – cefazolin 2 g or more or cefuroxime 1.5 g or more
In the current quarter, 98 percent of hip and knee arthroplasty procedures received the recommended antibiotic and dose. Nineteen of the twenty DHBs reached the threshold level of 95 percent compared with only three in the baseline quarter.[3]
SSII OS T 2
- Upper group: ≥ 95 percent
- Middle group: 90–94 percent
- Lower group: < 90 percent
Outcome marker: SSIs per 100 hip and knee operations
In quarter 4, 2018 there were 26 SSIs out of 2,583 hip and knee arthroplasty procedures, an SSI rate of 1.01 percent. A shift in the median is detected from August 2015, with the reduction being from 1.18 percent SSIs during the baseline period to 0.86 percent after it.
SSII OS T 3
SSI improvement – cardiac surgery
This is the ninth quality and safety marker (QSM) report for cardiac surgery. Since quarter 3, 2016 all five DHBs performing cardiac surgery have submitted process and outcome marker data from all cardiac surgery procedures, including coronary artery bypass graft with both chest and donor site, and with chest site only. There are three process markers and one outcome marker, which are similar to the markers for orthopaedic surgery.
Process marker 1: Timing – an antibiotic to be given 0–60 minutes before knife to skin
The target is 100 percent of procedures achieving this marker. Southern DHB achieved the target this quarter.
SSII - CS T 1
- Upper group: 100 percent
- Middle group: 95–99 percent
- Lower group: < 95 percent
Process marker 2: Dosing – correct antimicrobial prophylaxis used in at least 95 percent of procedures
The antibiotic prophylaxis of choice is to be ≥ 2 g or more of cefazolin for adults and ≥ 30 mg/kg of cefazolin for paediatric patients, not to exceed the adult dose. The target is that either dose is used in at least 95 percent of procedures. All DHBs performing cardiac surgery except Canterbury achieved the target this quarter.
SSII - CS T 2
- Upper group: > 95 percent
- Middle group: 90-95 percent
- Lower group: < 90 percent
Process marker 3: Skin preparation – appropriate skin antisepsis is always used
Appropriate skin antisepsis in surgery involves alcohol/chlorhexidine or alcohol/povidone iodine. The target is 100 percent of procedures achieving this marker. All DHBs except Southern achieved the target this quarter.
SSII - CS T 3
- Upper group: 100 percent
- Middle group: 95–99 percent
- Lower group: < 95 percent
Outcome marker: SSIs per 100 procedures rate
In quarter 4, 2018 we see the median shift downwards for the first time from 4.8 SSI cases per 100 cardiac procedures to 3.6. This is a significant improvement since the beginning of the Surgical Site Infection Improvement Programme. Cardiac surgical services in DHBs are dedicated to ensuring high compliance with the process measures in addition to implementing other quality improvement activities such as an anti-staphylococcal bundle.
SSII - CS T 4
Safe surgery
This is the 11th report for the safe surgery QSM, which measures levels of teamwork and communication around the paperless surgical safety checklist.
Direct observational audit was used to assess the use of the three surgical checklist parts: sign in, time out and sign out. A minimum of 50 observational audits per quarter per part is required before the observation is included in uptake and engagement assessments. Rates are greyed out in the tables below where there were fewer than 50 audits.
Figure 15 shows how many audits were undertaken for each part of the checklist. Thirteen out of the 20 DHBs achieved 50 audits for all three parts in quarter 1, 2019. Counties Manukau Health has a large auditor cohort, which explains its high numbers.
SS T 1
Rates for uptake (all components of the checklist were reviewed by the surgical team) are only presented where at least 50 audits were undertaken for a checklist part. Uptake rates were calculated by measuring the number of audits of a part where all components of the checklist were reviewed against the total number of audits undertaken.
The components for each part of the checklist are shown in the poster on the right. Of the 13 DHBs that achieved 50 audits in each checklist, seven achieved the 100 percent uptake target in at least one part of the checklist, during the current quarter (see Figure 16). Data is not presented where there were fewer than 50 audits.
SS T 2
The levels of team engagement with each part of the checklist were scored using a seven-point Likert scale developed by the World Health Organization. A score of 1 represents poor engagement from the team and 7 means team engagement was excellent. The target is that 95 percent of surgical procedures score engagement levels of 5 or above. As Figure 17 shows, for the latest quarter Bay of Plenty and Wairarapa DHBs achieved the target in all three parts. Twelve other DHBs achieved the target in one or two parts – an increase from nine DHBs last quarter. Data are not presented where there were fewer than 50 audits.
SS T 3
The safe surgery quality and safety domain now includes a start-of-list briefing measure to reinforce the importance of the briefing as a safe surgery intervention. The measure is described as ‘Was a briefing including all three clinical teams done at the start of the list?’
Figure 18 shows, in quarter 1, 2019, 13 DHBs reported that a start-of-list briefing was happening. There is no specific target for this part of the measure; the aim is to have all 20 DHBs increasingly undertaking and reporting briefings over time. The programme team continues to work with the auditing teams to increase data submission rates so the report better matches practice in DHBs.
SS T 4
The rates for postoperative sepsis and deep vein thrombosis/pulmonary embolism (DVT/PE) are the two outcome markers for safe surgery. The rates have fluctuated over time. To understand the factors driving the changes and to provide risk-adjusted outcomes in the monitoring and improvement of surgical QSMs, we have developed a risk-adjustment model for these two outcome markers.
The model is used to identify how likely patients being operated on were to develop sepsis or DVT/PE based on factors such as their condition, health history and the operation being undertaken. From this, we can calculate how many patients we would have predicted to develop sepsis or DVT/PE based on historic trends. We can then compare how many patients actually did develop sepsis or DVT/PE to create an observed/expected (O/E) ratio. If the O/E ratio is more than 1 then there are more sepsis or DVT/PE cases than expected, even when patient risk is taken into account. A ratio of less than 1 indicates fewer sepsis or DVT/PE cases than expected.
Figure 19 shows the DVT/PE risk-adjustment model results in two charts. Using the same methodology as above, the O/E ratio control chart shows there were 11 consecutive quarters in which the observed numbers were below the expected numbers since quarter 2, 2013. This indicates a statistically significant downwards shift, taking into account the increasing number of high-risk patients treated by hospitals and more complex procedures undertaken by hospitals. Over the past three years, a higher number of cases of DVT/PE have been observed in the second quarter.
SS T 5
Medication safety – electronic medicine reconciliation
This quality and safety domain focuses on medicine reconciliation where the process is supported with electronic data capture. Medicine reconciliation is a process by which health professionals accurately document all medicines a patient is taking and their adverse reactions history (including allergy). The information is then used during the patient’s transitions in care. An accurate medicines list can be reviewed to check the medicines are appropriate and safe. Medicines that should be continued, stopped or temporarily stopped can be documented on the list. Reconciliation reduces the risk of medicines being:
- omitted
- prescribed at the wrong dose
- prescribed to a patient who is allergic
- prescribed when they have the potential to interact with other prescribed medicines.
The introduction of electronic medicine reconciliation (eMedRec) allows reconciliation to be done more routinely, including at discharge. There is a national programme to roll out eMedRec throughout the country. Figures 20 and 21 show there are six DHBs that have implemented the system to date. Further uptake of eMedRec is limited until the IT infrastructure is improved in each DHB hospital.
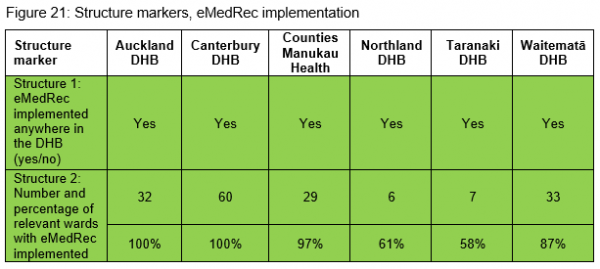
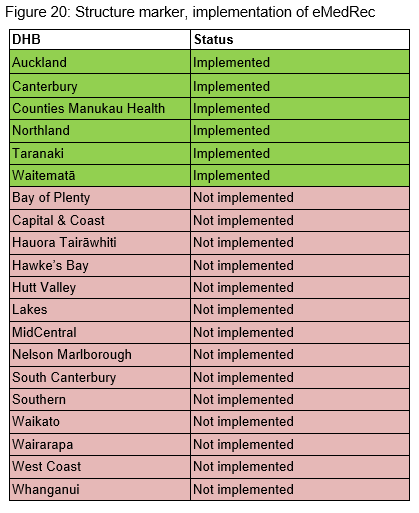

Within the six DHBs that have implemented eMedRec, only Northland and Taranaki DHB hospitals are reporting their process markers. Figure 22 shows the process marker change over time for these two DHBs. Further work is being undertaken on refining and agreeing the eMedRec marker definitions. Once this has been achieved the other DHB hospitals using eMedRec will report their process markers.
MS T 1
Patient deterioration
This is the fourth quarter that structural, process and outcome measures for the patient deterioration QSMs have been reported.
DHBs were asked to provide both process and outcome measure data by ethnicity where possible. Despite an increase in ethnicity data submitted from the previous quarter, we have not included this in the national report because the majority of DHBs were still unable to submit. We acknowledge that, for some DHBs, it will take more time to start collecting and submitting ethnicity-level data.
Structural measure: Eligible wards using the New Zealand early warning score
The structural measure demonstrates the progress DHBs have made towards implementing improvements to their recognition and response systems and aligning with the New Zealand early warning score (NZEWS).
The majority of DHBs (90 percent, n=18) have now implemented or are in the process of implementing the NZEWS in their hospitals. We have also seen an increase in the use of the tool across all eligible wards from the last quarter (now at 98 percent). Note: the New Zealand percentage is calculated based only on those DHBs that have implemented the NZEWS.
PD T 1
Process measure 1: Correct calculation of early warning score
The first process measure shows the percentage of audited patients with an early warning score calculated correctly for the most recent set of vital signs. This measure demonstrates how the recognition part of the system is working through the correct use of the NZEWS. We’ve introduced a threshold to indicate relative groupings for this quarter. Results for this measure show a national figure of 91 percent for this quarter.
19 DHBs (95 percent) submitted data for this measure. Those using an electronic vital signs system in all their eligible wards will be able to achieve 100 percent consistently for this measure. While Southern DHB is yet to implement the NZEWS, they have reported data using their existing EWS.
PD T 2
Process measure 2: Appropriate response to escalations
The second process measure shows the percentage of audited patients that triggered an escalation of care and received the appropriate response to that escalation as per the DHB’s agreed escalation pathway. This measure demonstrates how the response part of the system is working through the appropriate response to care that has been escalated.
The national figure for this measure was 65 percent, a decrease from the previous quarter. There was also considerably more variation between DHBs than for the first process measure, highlighting an opportunity for improvement. The Commission is currently working with DHBs to understand this variation, in particular regarding the consistency of data collected, the sample size and timeframes regarding the escalation pathway. A total of 18 DHBs (90 percent) submitted data for this measure.
PD T 3
Outcome measure 1: Rate of in-hospital cardiopulmonary arrests (preliminary results)
The following outcome measures will be used over time to determine whether the improvements to hospitals’ recognition and response systems have improved patient outcomes. Both measures are shown in a rate per 1,000 admissions. It is important to note that the preliminary admissions data used to calculate the rate is taken from the National Minimum Dataset (NMDS) at a DHB level and may differ from rates generated from administrative systems locally.
The results show a national rate of 1.3 cardiopulmonary arrests per 1,000 admissions for this quarter. Seventeen DHBs provided data for this measure. Canterbury DHB is not displayed this quarter because it is currently developing systems to capture cardiac arrest data.
PD T 4
Outcome measure 2: Rate of rapid response escalations (preliminary results)
The second outcome measure shows the rate of rapid response escalations per 1,000 admissions (excluding those mentioned previously). Consistent with the previous quarter, the results showed a national rate of 26 events per 1,000 admissions. Sixteen DHBs (80 percent) provided data for this measure.
International research has shown that an effective recognition and response system will result in an inverse relationship between outcome measures 1 and 2 (ie, a higher rate of rapid response escalations with a lower rate of in-hospital cardiopulmonary arrests). Another outcome measure used internationally is unplanned admissions to intensive care units. See the patient deterioration domain of the Atlas of Healthcare Variation for this data.
PD T 5
To further investigate the relationship between process measures 1 and 2 we have developed a scatterplot. The aim over time, is to have all DHBs locate in the top right corner which reveals a high rate of NZEWS scoring accuracy and appropriate response. It shows all DHBs that supplied data had a high rate of early warning score calculated correctly but there is more variation in the reported rates of appropriate response.
PD T 6
Pressure injury
We aim to reduce the occurrence of and harm from pressure injuries (PIs). PIs (also known as pressure ulcers, decubitus ulcers, pressure areas and bed sores) are a cause of preventable harm for people using health care services, including hospital, aged residential care and home or community care.
PIs are often avoidable, have significant negative impact on patient’s lives, whānau, and those providing their care, increase hospital length of stay and are associated with extra resource consumption.
Following implementation of the PI QSM in July 2018 the majority of DHBs (95 percent, n=19) are now submitting data. This is the first quarter that process and outcome measures have been reported publicly. Following review of data this quarter we are planning to engage with DHBs to better understand local data collection processes.
Process measure 1: percentage of patients with a documented and current pressure injury risk assessment
The first process measure shows the percentage of patients with a documented and current pressure injury risk assessment. This measure is used to monitor how well DHBs are conducting pressure injury risk assessments and recognising at-risk patients. This includes those at risk of developing a pressure injury and those with an existing pressure injury.
Results for this measure revealed a national figure of 81 percent.
A total of 19 DHBs (95 percent) submitted data for this measure.
PI T 1
Process measure 2: Percentage of at-risk patients with a documented and current individualised care plan
The second process measure shows the percentage of at-risk patients with a documented and current individualised care plan designed to address any risk (prevention) or manage any existing pressure injuries. This measure is used to monitor how well DHBs are putting in actions to prevent or manage pressure injuries for at-risk patients.
The national figure for this measure was a rate of 80 percent.
A total of 18 DHBs (90 percent) submitted data for this measure.
PI T 2
Outcome measure 1: Percentage of patients with hospital-acquired pressure injury
The following outcome measures will be used over time to determine whether the improvements to prevention and management of pressure injuries have improved patient outcomes.
The first outcome measure shows the percentage of patients with hospital-acquired pressure injuries (ie, pressure injuries that formed while the patient was in hospital).
The national figure for this measure was a rate of 3.5 percent. There is also considerable variation between DHBs highlighting an opportunity for improvement. We are working with DHBs to improve consistency of data collection.
A total of 18 DHBs (90 percent) submitted data for this measure.
PI T 3
Outcome measure 2: Percentage of patients with a non-hospital-acquired pressure injury
The second outcome measure shows the percentage of patients with non-hospital-acquired pressure injuries (ie, patients that arrived at hospital with a pressure injury that was formed in aged residential care, at home or in community care.)
The national figure for this measure was a rate of 1.4 percent. There is also considerable variation for this outcome measure highlighting an opportunity for improvement.
A total of 18 DHBs (90 percent) submitted data for this measure.
PI T 4
References
- de Raad J–P. 2012. Towards a value proposition: scoping the cost of falls. Wellington: NZIER.
- Ibid.
- In quarter 1, 2015, 1.5 g or more of cefuroxime was accepted as an alternative agent to 2 g or more of cefazolin for routine antibiotic prophylaxis for hip and knee replacements. This improved the results of this process measure for MidCentral DHB significantly, from 10 percent before the change to 96 percent immediately after the change. It also increased the national result from 90 percent to 95 percent in quarter 1, 2015.
