The goal of this Atlas domain is to highlight regional and demographic variation in the use of contraceptives.
Availability, affordability, acceptability and access to contraception information and services is a human right[1]. This Atlas domain is based on the principle that all available contraceptive choices should be obtainable by all women who need them in Aotearoa New Zealand.
The Atlas domain presents indicators showing available data on each contraceptive method. The indicators are presented in order of effectiveness of contraceptive method, with the most effective method first. For some methods the rates are low, reflecting either missing data (see comment below on data limitations) or low use. Where significant differences are reported, these are statistically significant using a 95 percent confidence interval.
Contraceptive use by women
This Atlas highlights low use of the most effective contraceptive methods. Despite their effectiveness and high patient satisfaction, the rate of long-acting reversible contraceptive (LARC) use was low.
| Indicator | Description (2018) | Number of women | Percent | New Zealand Health Survey findingsα |
| Women aged 10–54 living in Aotearoa NZ* | 1,467,375 | - | - | |
| 1 | Jadelle implant | 9,118 | 0.62 | 3.6 |
| 2 | IUS (mirena or jaydess) | 5,322 | 0.36 | 4.6 |
| X | IUD | Not known | - | 4.5 |
| X | DPMA | Not known | - | 4.4 |
| 3 | Female sterilisation (public only) (25–44) | 1,903 | 0.29 | 5.3 |
| 4 | Oral contraceptive | 217,187 | 14.8 | 17.5 |
| 5 | Regular oral contraceptive | 120,370 | 8.2 | - |
| X | Women relying on male vasectomy | Not known | - | 10.1 |
DMPA = depot-medroxyprogesterone acetate; IUD = intra-uterine device; IUS = intra-uterine system.
* Note: not all women of this age group will require contraception. The data for Jadelle, IUS and sterilisation is for 2018. However, these methods can last between three years to permanent (sterilisation). The data does not include some self-funded use.
α New Zealand Health Survey (2014/15). Contraceptive methods used (among women aged 16–49 years who had had vaginal sex in the four weeks preceding the survey).
Māori and Pacific women had higher rates of LARC (Jadelle) and sterilisation use than European/Other, however these rates were very low overall.
- In 2018, 0.62 percent of women received a Jadelle implant. Rates varied 2.8-fold between DHBs.
- A total of 0.36 percent of women were dispensed an IUS (Mirena or Jaydess). Rates varied three-fold between district health boards (DHBs).
- It was not possible to measure how many women used an IUD.
- In 2018, 0.29 percent of women aged 25–44 years were provided female sterilisation. Rates varied six-fold between DHBs.
- The most common method was the oral contraceptive with 14.8 percent of women aged 10–54 years dispensed the pill at least once.
- European/Other women aged 10–54 years were almost twice as likely to be dispensed an oral contraceptive (19 percent) compared with 11 percent of Māori, 7 percent of Asian and 6 percent of Pacific women.
- Use varied more than two-fold by DHB. In women aged 20–24 years rates varied from 19 percent to 49 percent.
- Of those aged 20–24 years, 18 percent received at least nine months’ supply of oral contraceptive in the year. The rate of regular contraceptive use reduced with age.
- Forty-seven percent of women received a LARC at a time of abortion. Rates varied almost two-fold between DHBs, from 33 percent to 62 percent of women of all ages.
- Ten percent of women were not provided with any contraception at time of abortion. DHB rates varied, even within narrow age bands. For example, the percentage of women aged 25–29 years who were not provided with any contraceptive ranged from 0 to 32 percent.
LARCs are one of the most effective and reliable forms of contraception.[1] The costs associated with LARCs are:
- initial appointment cost
- device cost
- the cost of the procedures to both insert and remove.
Even where a LARC is funded by PHARMAC, there may be a cost for the initial appointment and for insertion and subsequent removal. LARCs have a number of non-contraceptive benefits such as a reduction in menstrual bleeding and pain. They have high rates of satisfaction and 12-month continuation rates compared with the oral contraceptive pill.[2]
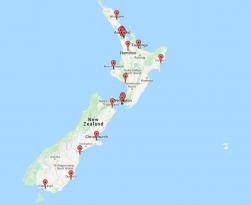
Figure 1: Location of Family Planning clinics in New Zealand in 2018
There are two types of intra-uterine contraception available: the progestogen-releasing IUS Mirena and Jaydess, and the non-hormonal copper IUD. All copper IUDs are dispensed via practitioner’s supply order (PSO), whereas around 99 percent of IUS are dispensed to people with a known NHI. IUS and IUD provide protection for up to five years. Since November 2019, the Mirena IUS device has been available fully funded by PHARMAC. Prior to this, funded use via Special Authority was limited to women with heavy menstrual bleeding and a ferritin (iron) level below 16 mcg. Community use has increased approximately five-fold since the IUS device became funded.
Research has concluded that ‘system and clinical barriers impact on young Māori mothers’ access to timely contraception despite these women actively seeking contraception. The lack of integration and limited funding formulas in the Aotearoa New Zealand public funded system results in multiple missed opportunities to meet these young women’s needs for effective contraception.’[2]
 Contraceptive use by women: key findings 2018 (click to download full size (115KB, pdf))
Contraceptive use by women: key findings 2018 (click to download full size (115KB, pdf))
In 2018, 0.6 percent of women (9,118) were dispensed a Jadelle implant
Jadelle implants are available through primary care or Family Planning clinics. This indicator includes data from community pharmacy dispensing and PSO from Family Planning. Our analysis suggests we are capturing most of the publicly funded provision in Aotearoa New Zealand in this time period. However, this may miss some dispensing, for example, Jadelle inserted postpartum (after giving birth).
- Rates in Māori and Pacific women were almost double those of non-Māori, non-Pacific women.
- There was 2.8-fold variation between DHBs in rates. DHBs with Family Planning clinics[3] tended to have higher rates.
- The map on the right shows the physical location of Family Planning clinics. This highlights that access can be an issue even in DHBs with the service.
In 2018, 0.4 percent of women aged 10–54 years were dispensed an IUS
- Use was highest in women aged 40–49 years, at 0.6 percent, and lowest in those aged 10–19 years (0.1 percent).
- Pacific and Asian women were less likely to be dispensed an IUS than Māori or European/Other women.
- Rates varied up to three-fold by DHB, from 0.2 percent to 0.6 percent of women aged 15–49 years.
Publicly funded female sterilisation was provided to 0.29 percent women aged 25–44 years in 2018
Female sterilisation is intended to provide permanent contraception.
- Rates were highest in those aged 35–39 years.
- Rates in Māori and Pacific women were significantly higher than Asian and European/Other women. It is possible that, if private procedures were included, rates would be higher in non-Māori, non-Pacific women.
- Age was limited to 25–44 years to remove women who may be undergoing female sterilisation for a reason other than contraception.
- Rates varied six-fold between DHBs from 0.13 percent to 0.84 percent.
Of women aged 10–54 years, 15 percent were dispensed an oral contraceptive in 2018
- Rates were highest in those aged 20–24 years at 30 percent.
- Rates varied two-fold between DHBs. Within the 20–24-year age band, there was significant regional variation: in the lowest DHB, 19 percent of women were dispensed an oral contraceptive compared with 49 percent in the highest DHB.
- There were marked ethnic differences. Overall, 19 percent of European/Other women aged 10–54 years were dispensed an oral contraceptive in 2018, compared with 11 percent of Māori, 7 percent of Asian and 6 percent of Pacific women.
Eight percent of women aged 10–54 years were regularly dispensed an oral contraceptive in 2018. Women of European/Other ethnicity were at least 2.5 times more likely to regularly receive an oral contraceptive than those of other ethnicities.
- Of those aged 20–24 years, 18 percent received at least nine months’ supply of oral contraceptive in 2018. The rate of regular contraceptive use reduced with age.
- Of women aged 10–54 years dispensed an oral contraceptive at least once in 2018, discontinuation rates were up to 45 percent.
- Rates of regular use were highest in those aged 20–24 years, at 18 percent, and lowest in those aged 10–14 years. Non-regular use may reflect discontinuation or women starting the pill part-way through the year. Discontinuation rates may reflect use of the pill for an indication other than contraception, unacceptable side effects, switching to an alternate method or barriers to access such as cost.
- Of those aged 15–19 years, European/Other women were 2.9 times more likely to regularly receive an oral contraceptive than Māori women, 8.3 times more likely than Pacific women and 6.4 times more likely than Asian women.
Percentage of women regularly dispensed an oral contraceptive, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | |||||||||
| 10–14 | 15–19 | 20–24 | 25–29 | 30–34 | 35–39 | 40–44 | 45–49 | 50–54 | Total | |
| Māori | 0.2 | 6.7 | 8.9 | 7.1 | 5.9 | 4.9 | 3.3 | 2.4 | 1.0 | 4.6 |
| Pacific peoples | 0.1 | 2.3 | 4.3 | 3.5 | 3 | 2.8 | 2.4 | 1.6 | 0.7 | 2.4 |
| Asian | 0.1 | 3.0 | 6.8 | 5.4 | 3.7 | 3.3 | 2.5 | 1.7 | 0.5 | 3.3 |
| European/Other | 0.5 | 19.2 | 26.5 | 18.2 | 12.7 | 11.2 | 8.3 | 5.1 | 1.9 | 11.4 |
| Total | 0.4 | 12.5 | 17.9 | 12.8 | 9.1 | 8 | 6.2 | 4 | 1.5 | 8.2 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
These findings should be interpreted in the context of women and their ability to access primary care. The health service access Atlas domain shows that 39 percent of 15–24-year-old women reported not visiting their GP or nurse at some point in 2019 due to cost compared with 26 percent of males in the same age group.
In 2018, 47 percent of women received a LARC at time of abortion
- Rates varied by ethnicity, with the highest being in Māori and Pacific women at 58 percent and 62 percent respectively, and the lowest being in Asian women at 36 percent.
- Women aged 40 years and over were less likely to receive a LARC (42 percent) than women aged under 40 years (48 percent).
- Between DHBs, rates varied almost two-fold. For all ages, LARC rates ranged between 33 percent to 62 percent of women.
- This indicator only includes first trimester abortions (until the end of the 14th week of pregnancy (1–12 weeks after conception, 0–104 days)).
Many women report using some form of contraception at the time of unintended pregnancy and the Choice study[4] showed that women were not always aware of failure rates and the effectiveness of different methods. The standards of care for women requesting abortion in Aotearoa New Zealand[5] (2018) note that abortion services play a very important role in preventing further unintended pregnancies. The standards specify that all women should have post-abortion contraception discussed with them beforehand, and supplies should be available or prescriptions given on the day of the abortion. LARCs are the most effective and reliable form of contraception.[6] Widespread availability of LARC is particularly important given the recent change in abortion law, intended to provide increased community provision of early medical abortion (EMA). A lack of access to funded LARC in the community combined with an increase in the rate of community EMA could lead to a rise in the number of repeat abortions.
Percentage of women receiving LARC at time of abortion, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | ||||||
| Under 20 | 20–24 | 25–29 | 30–34 | 35–39 | 40 or over | Total | |
| Māori | 58.4 | 53.7 | 59.0 | 60.4 | 58.6 | 54.8 | 57.4 |
| Pacific peoples | 57.6 | 59.3 | 65.3 | 62.5 | 61.1 | 47.6 | 60.8 |
| Asian | 33.0 | 25.9 | 30.1 | 43.2 | 42.8 | 41.6 | 35.6 |
| European/other | 42.4 | 48.5 | 47.7 | 38.8 | 38.4 | 34.4 | 43.6 |
| Total | 48.7 | 47.6 | 47.8 | 46.3 | 44.1 | 40.1 | 46.7 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
Ten percent of women did not receive any contraception at time of abortion in 2018
- Rates increased with age, with women 40 years and over less likely to receive contraception than younger women.
- DHB rates varied, even within narrow age bands. For example, the percentage of women aged 25–29 years not provided with any contraception ranged from 0 to 32 percent.
Percentage of women not receiving any contraception at time of abortion, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | ||||||
| Under 20 | 20–24 | 25–29 | 30–34 | 35–39 | 40 or over | Total | |
| Māori | 4.7 | 7.2 | 6.9 | 6.5 | 9.5 | 11.3 | 7.0 |
| Pacific peoples | 10.0 | 8.6 | 9.0 | 5.8 | 13.0 | 7.1 | 8.8 |
| Asian | 8.2 | 8.9 | 12.7 | 11.1 | 14.1 | 19.5 | 12.1 |
| European/other | 5.1 | 8.0 | 11.3 | 16.5 | 22.0 | 26.6 | 13.2 |
| Total | 5.9 | 8.0 | 10.4 | 12.2 | 17.3 | 21.3 | 11.1 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
Note: we cannot tell from the data whether women were offered contraception and declined it or if contraception was not offered.
- Do women in Aotearoa New Zealand have enough information on the effectiveness, risks and benefits of contraceptive methods?
- Are these methods equally available and accessible across Aotearoa New Zealand?
- How do women find out costs and providers of contraception in their region?
- How do the costs associated with insertion of LARCs influence women’s choice of contraception? How can this access barrier be addressed?
- How do women find out contraceptive options in your region? Is there enough information available for women to make a fully informed choice?
- What are you doing to ensure your communities have the information and options they need?
- What sources of funding are available within your DHB?
The World Health Organization, in its guidance document Ensuring human rights in the provision of contraceptive information and services,[7] sets out the following elements of quality of care in family planning:
- choice among a wide range of contraceptive methods
- evidence-based information on the effectiveness, risks and benefits of different methods
- technically competent, trained health workers
- provider–user relationships based on respect for informed choice, privacy and confidentiality
- the appropriate mix of services available in the same locality.
Click here to view the methodology
Data for this Atlas domain was drawn from the Pharmaceutical Collection, which contains claim and payment information from community pharmacists for subsidised dispensing. This does not include:
- prescription-only contraceptives provided directly via PSO or a bulk supply order (BSO)
- unsubsidised use of contraceptives, for example, women directly purchasing (for example, Mirena or Jaydess prior to November 2019, or condoms)
- copper IUD
- emergency contraception.
Data presented includes contraception used for con-contraceptive indications, for example, heavy menstrual bleeding or dysmenorrhoea. Finally, the data does not indicate whether people used the contraceptive after it was dispensed.
PSO means a practitioner has a supply of community pharmaceuticals, including contraceptive devices, that can be provided directly to patients. The pharmaceuticals are for emergency use, for teaching and demonstration purposes, and for provision to certain patient groups where an individual prescription is not practicable. In the context of contraceptives, the intention of PSO is to improve access to medicines to certain groups of women. However, a consequence of having a high proportion of a contraceptives dispensed via PSO is that data on who the contraceptive is supplied to is lost. This impacts on the ability to monitor access and uptake of contraceptives through quality measures.
This is of particular importance when considering the copper IUD. Used as emergency contraception (EC), its failure rate (0.1 percent) is far lower than the failure rate of oral emergency contraception (up to 15 percent), and it is considered the ‘gold standard’ method for this indication. However, due to barriers in access, including lack of trained practitioners and time constraints, it is rarely offered as EC in primary care. In order to monitor and encourage use of the copper IUD as EC, data collection will be required. This data collection, including practitioner discussions of LARC and documentation of methods accepted, has been incentivised in other countries such as the UK, leading to a high rate of uptake of LARC.[8]
The table below shows the proportion of a contraceptive dispensed to a known NHI against all dispensings of that contraceptive. A low percentage indicates that most of the contraceptive is accessed via PSO or BSO.
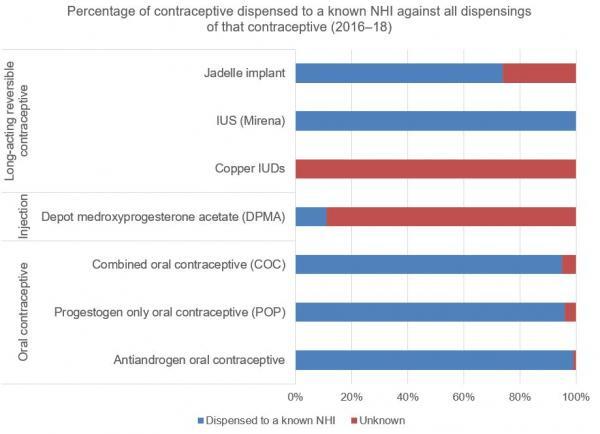
Source: Ministry of Health's Pharmaceutical Collection, extracted on 09 November 2020. See: https://tewhatuora.shinyapps.io/pharmaceutical-data-web-tool/
Chesang J, Richardson A, Potter, et al. 2016. Prevalence of contraceptive use in New Zealand women. NZMJ 129(1444): 71–80.
Lawton B, Makowharemahihi C, Cram F, et al. 2016. E Hine: access to contraception for indigenous Māori teenage mothers. J Prim Health Care. 8(1): 52–9.
EPiC Annual Prescribing Report includes data story on Contraceptive use by women. Published by He Ako Hiringa. Data current to last three months. Updated Annually. Practitioner, practice, and national data: https://epic.akohiringa.co.nz/annual-report
- United Nations. nd. Family planning. URL: www.unfpa.org/family-planning#:~:text=Access%20to%20safe%2C%20voluntary%20family%20planning
%20is%20a%20human%20right.&text=UNFPA%20works%20to%20support%20
family,data%20to%20support%20this%20work (accessed August 2020). - Lawton B, Makowharemahihi C, Cram F et al. E Hine: access to contraception for indigenous Māori teenage mothers. J Prim Health Care. 2016; 8(1): 52 – 59.
- There are 32 clinics in New Zealand, but there are not clinics in every DHB region. See: www.familyplanning.org.nz/clinics.
- McNicholas C, Tessa M, Secura G, et al. 2014. The Contraceptive CHOICE Project Round Up: what we did and what we learned. Clin Obstet Gynecol 57(4): 635–43.
- Standards Committee to the Abortion Supervisory Committee. 2018. Standards of Care for women requesting abortion in Aotearoa New Zealand. Report of a Standards Committee to the Abortion Supervisory Committee. Wellington: Ministry of Justice. URL: www.justice.govt.nz/assets/Standards-of-Care-2018.pdf.
- https://bpac.org.nz/2019/contraception/options.aspx
- World Health Organization. 2014. Ensuring human rights in the provision of contraceptive information and services: guidance and recommendations. Geneva: World health Organization. URL: https://apps.who.int/iris/bitstream/handle/10665/102539/9789241506748_
eng.pdf;jsessionid=DED3F00C9710C9A13B98C20836A4D6D7?sequence=1. - Ma R, Cecil E, Bottle A, et al. 2020. Impact of a pay-for-performance scheme for long-acting reversible contraceptive (LARC) advice on contraceptive uptake and abortion in British primary care: An interrupted time series study. PLoS Med 17(9): e1003333. https://doi.org/ 10.1371/journal.pmed.1003333.
Key findings (2018) | contraception used by women aged 10–54 years
This Atlas highlights low use of the most effective contraceptive methods. Despite their effectiveness and high patient satisfaction, the rate of long-acting reversible contraceptive (LARC) use was low.
| Indicator | Description (2018) | Number of women | Percent | New Zealand Health Survey findingsα |
| Women aged 10–54 living in Aotearoa NZ* | 1,467,375 | - | - | |
| 1 | Jadelle implant | 9,118 | 0.62 | 3.6 |
| 2 | IUS (mirena or jaydess) | 5,322 | 0.36 | 4.6 |
| X | IUD | Not known | - | 4.5 |
| X | DPMA | Not known | - | 4.4 |
| 3 | Female sterilisation (public only) (25–44) | 1,903 | 0.29 | 5.3 |
| 4 | Oral contraceptive | 217,187 | 14.8 | 17.5 |
| 5 | Regular oral contraceptive | 120,370 | 8.2 | - |
| X | Women relying on male vasectomy | Not known | - | 10.1 |
DMPA = depot-medroxyprogesterone acetate; IUD = intra-uterine device; IUS = intra-uterine system.
* Note: not all women of this age group will require contraception. The data for Jadelle, IUS and sterilisation is for 2018. However, these methods can last between three years to permanent (sterilisation). The data does not include some self-funded use.
α New Zealand Health Survey (2014/15). Contraceptive methods used (among women aged 16–49 years who had had vaginal sex in the four weeks preceding the survey).
Māori and Pacific women had higher rates of LARC (Jadelle) and sterilisation use than European/Other, however these rates were very low overall.
- In 2018, 0.62 percent of women received a Jadelle implant. Rates varied 2.8-fold between DHBs.
- A total of 0.36 percent of women were dispensed an IUS (Mirena or Jaydess). Rates varied three-fold between district health boards (DHBs).
- It was not possible to measure how many women used an IUD.
- In 2018, 0.29 percent of women aged 25–44 years were provided female sterilisation. Rates varied six-fold between DHBs.
- The most common method was the oral contraceptive with 14.8 percent of women aged 10–54 years dispensed the pill at least once.
- European/Other women aged 10–54 years were almost twice as likely to be dispensed an oral contraceptive (19 percent) compared with 11 percent of Māori, 7 percent of Asian and 6 percent of Pacific women.
- Use varied more than two-fold by DHB. In women aged 20–24 years rates varied from 19 percent to 49 percent.
- Of those aged 20–24 years, 18 percent received at least nine months’ supply of oral contraceptive in the year. The rate of regular contraceptive use reduced with age.
- Forty-seven percent of women received a LARC at a time of abortion. Rates varied almost two-fold between DHBs, from 33 percent to 62 percent of women of all ages.
- Ten percent of women were not provided with any contraception at time of abortion. DHB rates varied, even within narrow age bands. For example, the percentage of women aged 25–29 years who were not provided with any contraceptive ranged from 0 to 32 percent.
LARCs are one of the most effective and reliable forms of contraception.[1] The costs associated with LARCs are:
- initial appointment cost
- device cost
- the cost of the procedures to both insert and remove.
Even where a LARC is funded by PHARMAC, there may be a cost for the initial appointment and for insertion and subsequent removal. LARCs have a number of non-contraceptive benefits such as a reduction in menstrual bleeding and pain. They have high rates of satisfaction and 12-month continuation rates compared with the oral contraceptive pill.[2]

Figure 1: Location of Family Planning clinics in New Zealand in 2018
There are two types of intra-uterine contraception available: the progestogen-releasing IUS Mirena and Jaydess, and the non-hormonal copper IUD. All copper IUDs are dispensed via practitioner’s supply order (PSO), whereas around 99 percent of IUS are dispensed to people with a known NHI. IUS and IUD provide protection for up to five years. Since November 2019, the Mirena IUS device has been available fully funded by PHARMAC. Prior to this, funded use via Special Authority was limited to women with heavy menstrual bleeding and a ferritin (iron) level below 16 mcg. Community use has increased approximately five-fold since the IUS device became funded.
Research has concluded that ‘system and clinical barriers impact on young Māori mothers’ access to timely contraception despite these women actively seeking contraception. The lack of integration and limited funding formulas in the Aotearoa New Zealand public funded system results in multiple missed opportunities to meet these young women’s needs for effective contraception.’[2]
 Contraceptive use by women: key findings 2018 (click to download full size (115KB, pdf))
Contraceptive use by women: key findings 2018 (click to download full size (115KB, pdf))
In 2018, 0.6 percent of women (9,118) were dispensed a Jadelle implant
Jadelle implants are available through primary care or Family Planning clinics. This indicator includes data from community pharmacy dispensing and PSO from Family Planning. Our analysis suggests we are capturing most of the publicly funded provision in Aotearoa New Zealand in this time period. However, this may miss some dispensing, for example, Jadelle inserted postpartum (after giving birth).
- Rates in Māori and Pacific women were almost double those of non-Māori, non-Pacific women.
- There was 2.8-fold variation between DHBs in rates. DHBs with Family Planning clinics[3] tended to have higher rates.
- The map on the right shows the physical location of Family Planning clinics. This highlights that access can be an issue even in DHBs with the service.
In 2018, 0.4 percent of women aged 10–54 years were dispensed an IUS
- Use was highest in women aged 40–49 years, at 0.6 percent, and lowest in those aged 10–19 years (0.1 percent).
- Pacific and Asian women were less likely to be dispensed an IUS than Māori or European/Other women.
- Rates varied up to three-fold by DHB, from 0.2 percent to 0.6 percent of women aged 15–49 years.
Publicly funded female sterilisation was provided to 0.29 percent women aged 25–44 years in 2018
Female sterilisation is intended to provide permanent contraception.
- Rates were highest in those aged 35–39 years.
- Rates in Māori and Pacific women were significantly higher than Asian and European/Other women. It is possible that, if private procedures were included, rates would be higher in non-Māori, non-Pacific women.
- Age was limited to 25–44 years to remove women who may be undergoing female sterilisation for a reason other than contraception.
- Rates varied six-fold between DHBs from 0.13 percent to 0.84 percent.
Of women aged 10–54 years, 15 percent were dispensed an oral contraceptive in 2018
- Rates were highest in those aged 20–24 years at 30 percent.
- Rates varied two-fold between DHBs. Within the 20–24-year age band, there was significant regional variation: in the lowest DHB, 19 percent of women were dispensed an oral contraceptive compared with 49 percent in the highest DHB.
- There were marked ethnic differences. Overall, 19 percent of European/Other women aged 10–54 years were dispensed an oral contraceptive in 2018, compared with 11 percent of Māori, 7 percent of Asian and 6 percent of Pacific women.
Eight percent of women aged 10–54 years were regularly dispensed an oral contraceptive in 2018. Women of European/Other ethnicity were at least 2.5 times more likely to regularly receive an oral contraceptive than those of other ethnicities.
- Of those aged 20–24 years, 18 percent received at least nine months’ supply of oral contraceptive in 2018. The rate of regular contraceptive use reduced with age.
- Of women aged 10–54 years dispensed an oral contraceptive at least once in 2018, discontinuation rates were up to 45 percent.
- Rates of regular use were highest in those aged 20–24 years, at 18 percent, and lowest in those aged 10–14 years. Non-regular use may reflect discontinuation or women starting the pill part-way through the year. Discontinuation rates may reflect use of the pill for an indication other than contraception, unacceptable side effects, switching to an alternate method or barriers to access such as cost.
- Of those aged 15–19 years, European/Other women were 2.9 times more likely to regularly receive an oral contraceptive than Māori women, 8.3 times more likely than Pacific women and 6.4 times more likely than Asian women.
Percentage of women regularly dispensed an oral contraceptive, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | |||||||||
| 10–14 | 15–19 | 20–24 | 25–29 | 30–34 | 35–39 | 40–44 | 45–49 | 50–54 | Total | |
| Māori | 0.2 | 6.7 | 8.9 | 7.1 | 5.9 | 4.9 | 3.3 | 2.4 | 1.0 | 4.6 |
| Pacific peoples | 0.1 | 2.3 | 4.3 | 3.5 | 3 | 2.8 | 2.4 | 1.6 | 0.7 | 2.4 |
| Asian | 0.1 | 3.0 | 6.8 | 5.4 | 3.7 | 3.3 | 2.5 | 1.7 | 0.5 | 3.3 |
| European/Other | 0.5 | 19.2 | 26.5 | 18.2 | 12.7 | 11.2 | 8.3 | 5.1 | 1.9 | 11.4 |
| Total | 0.4 | 12.5 | 17.9 | 12.8 | 9.1 | 8 | 6.2 | 4 | 1.5 | 8.2 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
These findings should be interpreted in the context of women and their ability to access primary care. The health service access Atlas domain shows that 39 percent of 15–24-year-old women reported not visiting their GP or nurse at some point in 2019 due to cost compared with 26 percent of males in the same age group.
In 2018, 47 percent of women received a LARC at time of abortion
- Rates varied by ethnicity, with the highest being in Māori and Pacific women at 58 percent and 62 percent respectively, and the lowest being in Asian women at 36 percent.
- Women aged 40 years and over were less likely to receive a LARC (42 percent) than women aged under 40 years (48 percent).
- Between DHBs, rates varied almost two-fold. For all ages, LARC rates ranged between 33 percent to 62 percent of women.
- This indicator only includes first trimester abortions (until the end of the 14th week of pregnancy (1–12 weeks after conception, 0–104 days)).
Many women report using some form of contraception at the time of unintended pregnancy and the Choice study[4] showed that women were not always aware of failure rates and the effectiveness of different methods. The standards of care for women requesting abortion in Aotearoa New Zealand[5] (2018) note that abortion services play a very important role in preventing further unintended pregnancies. The standards specify that all women should have post-abortion contraception discussed with them beforehand, and supplies should be available or prescriptions given on the day of the abortion. LARCs are the most effective and reliable form of contraception.[6] Widespread availability of LARC is particularly important given the recent change in abortion law, intended to provide increased community provision of early medical abortion (EMA). A lack of access to funded LARC in the community combined with an increase in the rate of community EMA could lead to a rise in the number of repeat abortions.
Percentage of women receiving LARC at time of abortion, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | ||||||
| Under 20 | 20–24 | 25–29 | 30–34 | 35–39 | 40 or over | Total | |
| Māori | 58.4 | 53.7 | 59.0 | 60.4 | 58.6 | 54.8 | 57.4 |
| Pacific peoples | 57.6 | 59.3 | 65.3 | 62.5 | 61.1 | 47.6 | 60.8 |
| Asian | 33.0 | 25.9 | 30.1 | 43.2 | 42.8 | 41.6 | 35.6 |
| European/other | 42.4 | 48.5 | 47.7 | 38.8 | 38.4 | 34.4 | 43.6 |
| Total | 48.7 | 47.6 | 47.8 | 46.3 | 44.1 | 40.1 | 46.7 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
Ten percent of women did not receive any contraception at time of abortion in 2018
- Rates increased with age, with women 40 years and over less likely to receive contraception than younger women.
- DHB rates varied, even within narrow age bands. For example, the percentage of women aged 25–29 years not provided with any contraception ranged from 0 to 32 percent.
Percentage of women not receiving any contraception at time of abortion, by age group and ethnicity (2018)
| Ethnicity | Age group (years) | ||||||
| Under 20 | 20–24 | 25–29 | 30–34 | 35–39 | 40 or over | Total | |
| Māori | 4.7 | 7.2 | 6.9 | 6.5 | 9.5 | 11.3 | 7.0 |
| Pacific peoples | 10.0 | 8.6 | 9.0 | 5.8 | 13.0 | 7.1 | 8.8 |
| Asian | 8.2 | 8.9 | 12.7 | 11.1 | 14.1 | 19.5 | 12.1 |
| European/other | 5.1 | 8.0 | 11.3 | 16.5 | 22.0 | 26.6 | 13.2 |
| Total | 5.9 | 8.0 | 10.4 | 12.2 | 17.3 | 21.3 | 11.1 |
Bold denotes European/Other significantly higher than other ethnic groups at each age band.
Note: we cannot tell from the data whether women were offered contraception and declined it or if contraception was not offered.
Questions the data prompts
- Do women in Aotearoa New Zealand have enough information on the effectiveness, risks and benefits of contraceptive methods?
- Are these methods equally available and accessible across Aotearoa New Zealand?
- How do women find out costs and providers of contraception in their region?
- How do the costs associated with insertion of LARCs influence women’s choice of contraception? How can this access barrier be addressed?
- How do women find out contraceptive options in your region? Is there enough information available for women to make a fully informed choice?
- What are you doing to ensure your communities have the information and options they need?
- What sources of funding are available within your DHB?
Background
The World Health Organization, in its guidance document Ensuring human rights in the provision of contraceptive information and services,[7] sets out the following elements of quality of care in family planning:
- choice among a wide range of contraceptive methods
- evidence-based information on the effectiveness, risks and benefits of different methods
- technically competent, trained health workers
- provider–user relationships based on respect for informed choice, privacy and confidentiality
- the appropriate mix of services available in the same locality.
Data limitations
Click here to view the methodology
Data for this Atlas domain was drawn from the Pharmaceutical Collection, which contains claim and payment information from community pharmacists for subsidised dispensing. This does not include:
- prescription-only contraceptives provided directly via PSO or a bulk supply order (BSO)
- unsubsidised use of contraceptives, for example, women directly purchasing (for example, Mirena or Jaydess prior to November 2019, or condoms)
- copper IUD
- emergency contraception.
Data presented includes contraception used for con-contraceptive indications, for example, heavy menstrual bleeding or dysmenorrhoea. Finally, the data does not indicate whether people used the contraceptive after it was dispensed.
PSO means a practitioner has a supply of community pharmaceuticals, including contraceptive devices, that can be provided directly to patients. The pharmaceuticals are for emergency use, for teaching and demonstration purposes, and for provision to certain patient groups where an individual prescription is not practicable. In the context of contraceptives, the intention of PSO is to improve access to medicines to certain groups of women. However, a consequence of having a high proportion of a contraceptives dispensed via PSO is that data on who the contraceptive is supplied to is lost. This impacts on the ability to monitor access and uptake of contraceptives through quality measures.
This is of particular importance when considering the copper IUD. Used as emergency contraception (EC), its failure rate (0.1 percent) is far lower than the failure rate of oral emergency contraception (up to 15 percent), and it is considered the ‘gold standard’ method for this indication. However, due to barriers in access, including lack of trained practitioners and time constraints, it is rarely offered as EC in primary care. In order to monitor and encourage use of the copper IUD as EC, data collection will be required. This data collection, including practitioner discussions of LARC and documentation of methods accepted, has been incentivised in other countries such as the UK, leading to a high rate of uptake of LARC.[8]
The table below shows the proportion of a contraceptive dispensed to a known NHI against all dispensings of that contraceptive. A low percentage indicates that most of the contraceptive is accessed via PSO or BSO.

Source: Ministry of Health's Pharmaceutical Collection, extracted on 09 November 2020. See: https://tewhatuora.shinyapps.io/pharmaceutical-data-web-tool/
Recommended reading
Chesang J, Richardson A, Potter, et al. 2016. Prevalence of contraceptive use in New Zealand women. NZMJ 129(1444): 71–80.
Lawton B, Makowharemahihi C, Cram F, et al. 2016. E Hine: access to contraception for indigenous Māori teenage mothers. J Prim Health Care. 8(1): 52–9.
EPiC Annual Prescribing Report includes data story on Contraceptive use by women. Published by He Ako Hiringa. Data current to last three months. Updated Annually. Practitioner, practice, and national data: https://epic.akohiringa.co.nz/annual-report
References
- United Nations. nd. Family planning. URL: www.unfpa.org/family-planning#:~:text=Access%20to%20safe%2C%20voluntary%20family%20planning
%20is%20a%20human%20right.&text=UNFPA%20works%20to%20support%20
family,data%20to%20support%20this%20work (accessed August 2020). - Lawton B, Makowharemahihi C, Cram F et al. E Hine: access to contraception for indigenous Māori teenage mothers. J Prim Health Care. 2016; 8(1): 52 – 59.
- There are 32 clinics in New Zealand, but there are not clinics in every DHB region. See: www.familyplanning.org.nz/clinics.
- McNicholas C, Tessa M, Secura G, et al. 2014. The Contraceptive CHOICE Project Round Up: what we did and what we learned. Clin Obstet Gynecol 57(4): 635–43.
- Standards Committee to the Abortion Supervisory Committee. 2018. Standards of Care for women requesting abortion in Aotearoa New Zealand. Report of a Standards Committee to the Abortion Supervisory Committee. Wellington: Ministry of Justice. URL: www.justice.govt.nz/assets/Standards-of-Care-2018.pdf.
- https://bpac.org.nz/2019/contraception/options.aspx
- World Health Organization. 2014. Ensuring human rights in the provision of contraceptive information and services: guidance and recommendations. Geneva: World health Organization. URL: https://apps.who.int/iris/bitstream/handle/10665/102539/9789241506748_
eng.pdf;jsessionid=DED3F00C9710C9A13B98C20836A4D6D7?sequence=1. - Ma R, Cecil E, Bottle A, et al. 2020. Impact of a pay-for-performance scheme for long-acting reversible contraceptive (LARC) advice on contraceptive uptake and abortion in British primary care: An interrupted time series study. PLoS Med 17(9): e1003333. https://doi.org/ 10.1371/journal.pmed.1003333.
